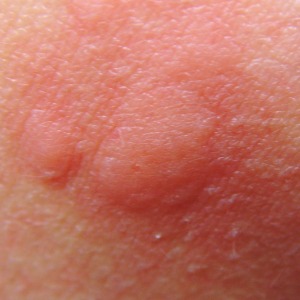
Malaria is a disease caused by a protozoan parasite that invades the red blood cells through the bite of infected mosquitoes. The parasite is transmitted by mosquitoes in many subtropical and tropical regions that kill an estimated 660,000 people each year. What does malaria look like on the skin? Initially, it may appear as any other mosquito bite, but if it becomes an itchy rash resembling hives, or severely itchy skin lesions marked by the appearance of smooth, slightly elevated papules, it may be an early marker of malaria.
Malaria: Causes and Means of Transmission
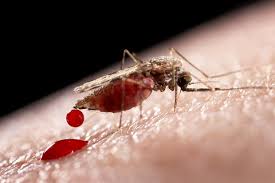
Only female Anopheles mosquitoes can transmit the disease, and they must also have been infected through a previous blood meal taken from a malaria infected person. If a mosquito infected with the Plasmodium parasite bites you, malaria can occur. An infected mother can also pass the disease (congenital malaria) to her infant at birth. Malaria is a blood borne disease, so it may also be transmitted through blood transfusion, organ transplant or shared needles.
Risk Factors
The largest risk factor for developing malaria is to live in, or visits to tropical areas where the disease is a common occurrence. Many different sub-types of malaria parasites exist. However, the type that causes the most lethal complications is found most commonly in:
- Papua New Guinea, Solomon Islands, and Haiti
- African countries south of the Sahara Desert
- The Asian subcontinent
Symptoms of Malaria
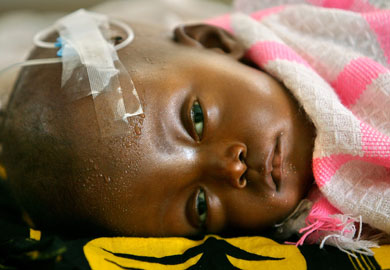
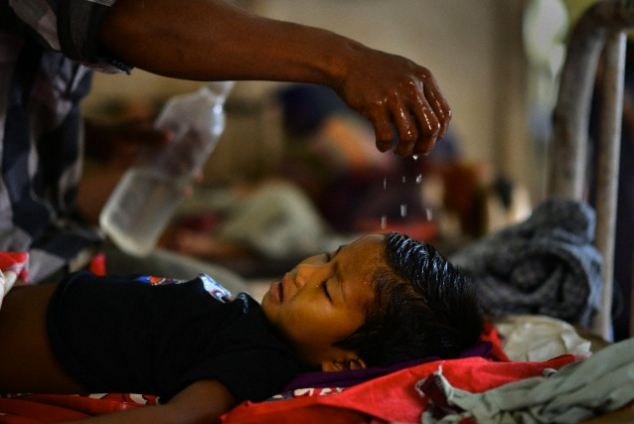
What does malaria look like on the skin? Malaria has a wide array of symptoms, not just on the skin. After the infected mosquito bite occurs, it may take between 7-30 days of incubation before any symptoms are noticed.
Uncomplicated Malaria
The most common symptoms are usually:
- Nausea and vomiting
- Chills with fever
- Body aches and general weakness
- Jaundice (yellow coloring of the eyes and skin) because of the loss of red blood cells
A classic description of an attack of malaria would be a 6-to-12-hour period of fever and headaches alternating with cold and shivering, to a stage of sweating and general weakness, and because the symptoms are very non-specific, it is important to determine if you have other risk factors for malaria such as travel in areas where the disease is common.
Severe (Complicated) Malaria
Complicated malaria occurs when other body systems are affected, such as:
- Kidney failure
- Cardiovascular collapse
- Severe anemia due to destruction of red blood cells
- Cerebral malaria (confusion or abnormal behavior, seizures, unconsciousness)
- Low blood sugar in pregnant women after treatment with quinine
How Malaria Is Diagnosed
Your physician may suspect that you have malaria based on your symptoms and your travel history. During physical examination, your physician may find an enlarged spleen as the result of malaria infection.
To confirm the diagnosis, your physician will take blood samples that have been treated with special chemicals in a laboratory to be examined for the Plasmodium parasites. In addition, blood tests will also determine whether malaria has affected your blood chemistry, such as the levels of red blood cells and platelets, the clotting ability of your blood, along with liver and kidney functions.
Treatment for Malaria
Know that you know the answer to “What does malaria look like on the skin?” let’s look at possible treatment options. Malaria is a life-threatening condition, and treatment for the disease is typically provided in a hospital setting. With proactive treatment, the symptoms of malaria can be cured quickly, usually in about 2 weeks. Without treatment, malaria can return occasionally over a number of years, and repeated exposure may cause some people to become partially immune, developing only a milder case of the disease.
The length of treatment and types of drugs will vary, depending on:
- Your age
- The severity of your symptoms
- Which type of malaria parasite you have
- Whether you're pregnant
- The most common antimalarial drugs include:
- Quinine sulfate (Qualaquin)
- Mefloquine
- Chloroquine (Aralen)
- Hydroxychloroquine (Plaquenil)
- Combination of atovaquone and proguanil (Malarone)
In some cases, the prescribed medication will not clear you from the infection. Some parasites that are resistant to drugs have been reported, and these parasites make many drugs ineffective. If this happens, your physician might need to use more than one medication or change medications in order to treat the condition.
Preventing Malaria
Medical experts are researching a vaccine against malaria, and the eventual vaccination is expected to be an important way to prevent malaria in the future. Other ways to prevent malaria is avoiding the mosquito using the following strategies:
- Wear clothing that covers most of your body, and apply insect repellent with permethrin to clothing.
- Apply an insect repellent that contains DEET or Picaridin to the exposed areas of your skin, except around your mouth and eyes.
- When possible, stay indoors, or in well-screened areas, especially in the evenings when the mosquitoes are most active.
- Use bed nets and mosquito nets when sleeping, and treat the nets with permethrin.
Medication
If you're travelingg to areas where malaria is common, in addition to knowing “What does malaria look like on the skin? ” it’s also recommended that you use preventive medicine before, during and after your trip.The most commonly prescribed anti-malarial medications in the U.S. include:
- Chloroquine (Aralen): commonly prescribed anti-malarial drug in countries where there are no drug-resistant strains of malaria. This medication is taken once weekly, from 1-2 weeks prior to travel, until a month after you’ve returned.
- Mefloquine (Lariam): for travel to most regions and areas that have evidence of chloroquine-resistant malaria parasites, such as sub-Saharan Africa. This medication is taken once weekly, from 1-2 weeks before travell until a month after your return.
- Doxycycline (Vibramycin): for people who cannot take chloroquine or mefloquine. Doxycycline is taken once daily, from 2 days before traveling to a month after you’ve returned.
- Atovaquone and proguanil (Malarone): for the protection from chloroquine-resistant malaria. You take one tablet at the same time daily, beginning 1-2 days before traveling until a week after you return.
- Primaquine: is used upon your return if you’ve stayed for more than a few months in an area where you had heavy exposure to mosquitoes. Primaquine is taken daily for 2 weeks after you have left the area.
If you develop an illness with fever within a year of your return, seek immediate medical attention and tell a healthcare provider about your travel.
