A transmetatarsal amputationmay be carried out to treat gangrene, and neurotrophic ulcerations. The procedure has long been preferred as an substitute for below-the-knee- amputations, with hope of salvaging both the threatened ischemic, as well as the neuropathic limbs. The procedure was first performed in the year 1855, as the treatment of trench foot, and there are reports that date back to 1949, which state a satisfactory result in over 67% (currently 77%) of patients who had undergone the procedure in treatment of gangrene and neurotrophic ulcerations. This article will explain all that you need to know about the procedure; including how and when it is performed.
What Is Transmetatarsal Amputation?
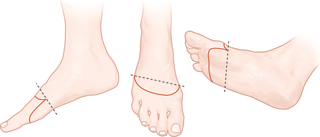
Transmetatarsal amputation (TMA) is a surgical procedure carried out to remove all, or part of the patient's forefoot, which includes the metatarsal bones—the five long bones between your ankle and toes. The operation is generally only performed when the area is infected or badly injured, meaning the blood vessels, tissue, boneand other parts of the forefoot are damaged beyond repair.
When Should Transmetatarsal Amputation Be Operated?
Before suggesting or performing the operation, the heathcare provider must first assess the patient's vascular adequacy, which can directly affect a patient's ability to heal efficiently after the amputation.
There are numerous conditions, such as diabetes, that can cause poor blood flow to an individual's foot; in such cases doctors may suggest a TMA. A TMA may also be the final solution in treatment of a damaged forefoot, when all treatment options have proven ineffective.Some conditions will indicate the need for a TMA. Several clinical indications are as follows:
- Chronic ulceration of the forefoot
- Gangrene of the forefoot (multiple digits)
- A combination of the above conditions (possibly complicated by diabetes mellitus)
- A severely crushed forefoot
Some contraindications for transmetatarsal amputation include:
- Tracking proximal infection (cellulitis, for example)
- Lymphangitis
How Is Transmetatarsal Amputation Operated?
1. Prepare for the Operation
Before the procedure, you must give your formal consent, by signing legal documentation—known as informed consent. This is to ensure that you know everything that you need to know about the procedure, to be able to weigh your options and decide whether you wish it to be carried out or not.You obtain the right to comprehend the medical care that you will be receiving, in words you know. Ensure that you understand the positives and negatives, as well as the risks associated with the procedure before signing over your consent.
Before the procedure starts, an IV will be placed into your vein to supply your body with liquid or medicine.Anesthesia will often be given before the procedure takes place, which anesthesia is best for you will likely be discussed with your doctor. Two main types being:
- General anesthesia: This medicine will ensure that you remain asleep during the procedure, and free from pain. Although this is often administered via an IV, it can also be breathed in through a mast, or via a tube placed down the throat—this method may cause a sore throat when you awaken.
- Spinal or epidural anesthesia: This medicine works to numb the area and dull the pain. You may still feel some pressure of pushing while the surgery takes place.
2. Perform the Operation
The surgeon will make deep incisions on your forefoot, and remove any damaged or infected bones. The blood vessels, tendons and nerves will be cut and sealed off. Your health care provider will then remove any remaining dead or infected tissue and continue to clean the inside of your foot.
If the infection within your forefoot is extremely severe, the incision will be left open and the wound packed with medical bandages. If the forefoot no longer shows signs of infection, the incision will be sealed with staples or stitches. On some occasions, a skin graph may be applied to cover the wound. Your health care provider may also administer one or more drains, in order to remove any extra fluid and/or blood from the wound. Bandages will be used to cover the wound and help to prevent bleeding, as well as inflammation.
3. Follow-Up Care
After the surgery, you will be taken to a resting room until you have fully awoken. It is imperative that you do not stand until your doctor says it is alright to. Your doctor will closely monitor you to ensure no post-surgical problems have arisen. Once it has been determined safe, you will be able to return home. Some important things to remember are:
- Take recovery exercise with professional help. You may need to walk the same day on surgery, or at least the day after. Although restingseems to be the best option for recovery, movement will help to prevent blood from clotting. You may also be provided with specialized exercises to practice in bed. Yet, you should not try to walk until your doctor permits you to do so, and ensure to converse with them before attempting to stand for the first time.
- Utilize assistive devices. You may require the use of crutches or a wheelchair to assist you with motion until your health care provider informs you that you are safe to put pressure on your foot again. And remember to use these devices as the professional instructs.
- Gradually build up your diet after surgery. You will likely first consume only liquids, such as water, broth and juice. If your stomach does not have any adverse reaction, then you may consume soft foods, such as applesauce or ice cream. Once you find the consumption of soft foods easy and without difficulty, then you may begin to incorporate solid foods back into your diet.
- Physical therapy sessions may help. You can take the physical therapy sessions to teach you exercises which help to increase strength, as well as reduce pain.
- Seek support from external devices. In some instances, you may need a splint or cast.This may be required to offer increased protection to the wound. Usually, shoe modifications are required. You can wear specialized footwear, with an extended foot plate and reduced peak plantar pressure.
Risks of Transmetatarsal Amputation
Risks associated with this procedure include:
- Bleeding
- The formation of blood clots in the legs, which may travel to the lungs, leading to breathing problems
- Phantom sensation—a feeling that the amputated limb is still there
- Joint contracture—joint near affected area looses full range of motion
- Skin or bone infections
- Insufficient healing of the surgical wound
When to Call Your Doctor
It is important that you check the site of amputation twice daily for any signs or further complications. Always call your doctor if any of the following occur:
- A rise in redness or warmth at the site of amputation, or red streaks of skin extending from the site.
- Bulging/swelling at the site of incision.
- New bleeding or leakage from your wound, or gaps between the stitches where the skin is pulling apart.
- The skin around the site of incision is becoming dark, or turning black.
- A temperature exceeding 101.5°F (38.5°C).
