Myasthenia gravis is a chronic disease characterized by progressive weakness and fatigue of the voluntary muscles. It is caused by an abnormal breakdown in communication between your muscles and nerves. Although it can affect people of any age, it is commonly seen in females below the age of 40 and in males above the age of 60. While there is no cure, treatment for myasthenia gravis helps relieve its signs and symptoms. A myasthenia gravis diagnosis can be made after your doctor reviews your medical history, conducts a physical examination and performs some laboratory tests.
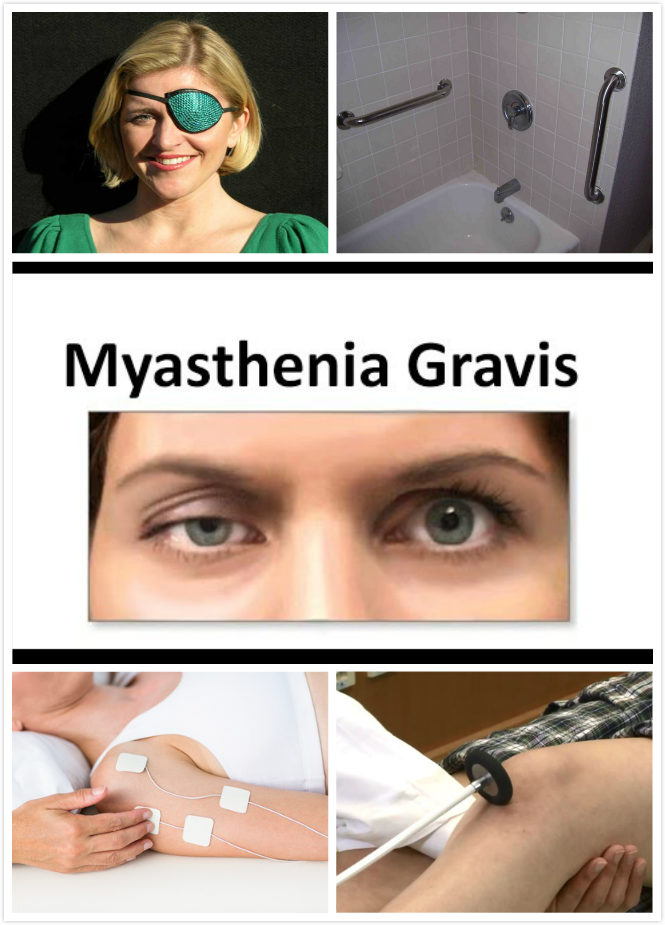
Diagnosis of Myasthenia Gravis
Myasthenia gravis is arare autoimmune disease characterized by skeletal muscle weakness. This chronic and progressive disorder causes your voluntary muscles to become weaker without thinning out (atrophy). To make a myasthenia gravis diagnosis, your doctor will examine you thoroughly and do some tests:
1. Neurological Examination
After your doctor takes your medical history which includes your signs and symptoms, he will conduct a neurologic examination to test your:
- balance
- coordination
- muscle strength
- muscle tone
- reflexes
- sense of sight and touch
2. Edrophonium Test
This involves the injection of a chemical called edrophonium chloride which usually results in a sudden, but temporary improvement of muscle strength. If positive, it indicates a myasthenia gravis diagnosis. However, this test has some side effects, including breathing problemsand rapid heart rate. It should be performed by experienced neurologists and must be done in centers whereresuscitation equipment is available. Therefore, it is often done when other tests are doubtful or negative.
3. Ice Pack Test
This is often done to replace the edrophonium test. People who have myasthenia gravis usually have droopy eyelids. Your doctor may use the test by placing a bag of ice on the eyelids for two minutes. Upon removal of the ice pack, he will analyze your eyelids for improvement.
4. Blood Analysis
A blood analysis may be used to check if there are abnormal proteins (antibodies) which cause the disruption of the receptor sites for chemicals involved in transmitting nerve impulses responsible for making your muscles move.
5. Nerve Stimulation
This test evaluates your muscles for fatigue. People who have myasthenia gravis experience muscle fatigue during repeated nerve stimulation because of the decline in the transmission of signals between nerves and muscles. In this test, your doctor will connect electrodes to the skin over your muscles. Small pulses of electricity are sent to evaluate the nerves’ capacity to send signals to the muscles. A myasthenia gravis diagnosis can be made when repetitive nerve stimulation worsens muscle fatigue.
6. Electromyography (EMG)
Electromyography is a test that helps identify any communication problems between a nerve and a muscle. It involves a fine needle electrode being inserted into a muscle, which records muscle activity. With myasthenia gravis, your muscle does not respond adequately to nerve stimulation.
7. Imaging Scans
A CT scan or MRI may be requested to check if you have a tumor or other abnormalities in your thymus. The thymus is a small gland which is found in the upper chest and is often associated with myasthenia gravis.
8. Pulmonary Function Tests
Pulmonary function tests may be needed to evaluate if your condition influences your respiratory function.
Symptoms of Myasthenia Gravis
Myasthenia gravis diagnosis should be correct if you have the following symptoms:
1. Eyes, Eyelids and Face
People with myasthenia gravis usually have one or two droopy eyelids (ptosis) which get worse in the afternoon. Changes in vision may also occur. In some patients, eye muscle abnormality is the only indication of the disease (ocular myasthenia). If your facial muscles are involved, your facial expression may become affected, sometimes producing a “snarling smile”.
2. Swallowing and Breathing
You may have difficulty in chewing, swallowing and breathing if the muscles of your tongue and mouth are affected. Your voice may become husky or you may develop a nasal voice. Coughing, choking and frequent chest infections may also develop. Some patients experience breathing difficulties, especially after exercise or when they lie flat in bed. If you develop severe breathing or swallowing problems, you may need urgenthospital admission for medical care.
3. Limb Movement
Myasthenia gravis can cause mobility problems, such as head drop, waddling gait and difficulty performing ordinary tasks such as:
- lifting
- washing hair
- brushing teeth
- climbing stairs
- rising from a sitting position
Even ordinary physical activities often lead to tiredness because of muscle weakness.
Home Remedies for Myasthenia Gravis
1. Change Eating Routine
Try eating early in the morning when your muscle has adequate strength. Take time to chew food and take frequent breaks between bites. Eat frequent and small meals. Also, eat soft food and avoid those that require a lot of chewing, like raw fruits and vegetables.
2. Install Safety Precautions
To be safe, install railings or grab bars in your home to provide support, especially near the bathtub or stairs. Keep floors clean and remove loose rugs. Keep your pathways, driveways and sidewalks clear.
3. Try an Eye Patch
Use an eye patch to relieve double vision, especially while writing or watching television. Switch eye patch between eyes periodically to reduce eyestrain.
Medical Treatments for Myasthenia Gravis
1. Medications
Treatment for myasthenia gravis consists of medications to relieve symptoms, but not to cure the disease. Pyridostigmine (Mestinon) may be prescribed to increase the amount of neurotransmitter available in the receptors for nerve stimulation. You may also need a steroid like prednisone and other drugs like azathioprine, mycophenolate and cyclosporine to suppress your immune system.
2. Plasma Exchange
For severe cases, plasma exchange (plasmapheresis) may be needed to remove the antibodies from your plasma and replace it with antibody-free plasma. You may also receive intravenous immunoglobulin.
3. Thymus Removal
Patients who have a tumor in their thymus (thymoma) will need surgery (thymectomy). Some doctors recommend this surgery even if there is no tumor present because it usually leads to improvement of symptoms in most patients.
4. Hospital Admission
Medical care in a hospital may be necessary if you have severe muscle weakness that causes difficulty breathing. During a severe infection, you may need treatment with antibiotics to avoid a myasthenic crisis.
