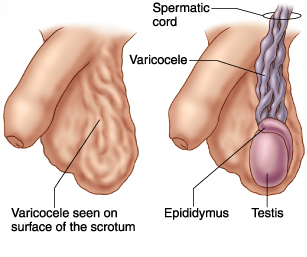
A varicocele is a common condition that affects males and is characterized by the enlargement of veins inside the scrotum, or the skin that holds the testicles (testis). It is similar to varicose veins found in the legs.
A varicocele occurs when the pampiniform veins, which form a network of small veins in the spermatic cord, become dilated. It appears and feels like a mass or a bag of worms around the testis. Varicocele ultrasound or Doppler ultrasonography will allow accurate diagnosis of the condition.
Varicocele Symptoms
 No signs and symptoms are usually experienced. Varicocele rarely causes pain, but if present, it may be experienced as a dull discomfort or a sharp pain. This may be intensified when standing or exercising for long periods. The pain may worsen during the day, but is relieved when lying on your back.
No signs and symptoms are usually experienced. Varicocele rarely causes pain, but if present, it may be experienced as a dull discomfort or a sharp pain. This may be intensified when standing or exercising for long periods. The pain may worsen during the day, but is relieved when lying on your back.
Varicoceles may become larger and more noticeable with time. Its presence can lead to impairment of sperm production, which can be improved with proper treatment.
Varicocele Diagnosis and Grading
A skilled physician may be able to diagnose varicocele diagnosis by obtaining the patient’s history and performing a thorough physical examination. To confirm the diagnosis, varicocele ultrasoundcombinedwith color flow Doppler may be done. Other methods to confirm the diagnosis also include scintigraphy, infrared thermography, venography, and magnetic resonance imaging.
Ultrasound examination begins with the patient lying supine with legs spread apart. The scrotum is supported by a sling to facilitate proper exposure while the penis is covered by a towel and secured to the abdomen with tape.
Varicocele ultrasound with color flow Doppler capability is used because it can accurately detect the condition with high sensitivity and specificity. A varicocele appears sonographically as multiple, wormlike, tubular structures representing the dilated veins. Normally, the pampiniform veins measure from 0.5 - 1.5 mm, but with varicocele, the diameters may range between 2 - 3 mm. When the patient is instructed to do a Valsalva maneuver, by forcibly exhaling while keeping the mouth and nose closed, venous flow in the varicocele will demonstrate retrograde filling and phasic variation.
Varicocele Ultrasound and Sonography Pictures
Varicocele ultrasound can help reliably diagnose the condition by demonstrating dilation of the pampiniform plexus of veins to more than 2 mm. A Valsalva maneuver or standing up during examination increases venous pressure, which will result in an increase in the dilatation of these veins. Here are some pictures to demonstrate varicocele by ultrasonography:
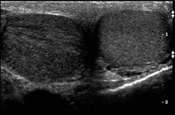
Transverse scanning of both testicles shows a normal left testicle compared to a right hypoechogenic (light) testicular torsion. (photo by Michael Blaivas, M.D.)
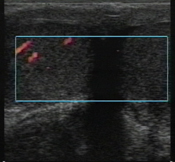
Varicocele ultrasound with color flow Doppler shows normal perfusion in the patient’s right testicle, but the left testicle, which is swollen, is not perfused. (photo by Michael Blaivas, M.D.)
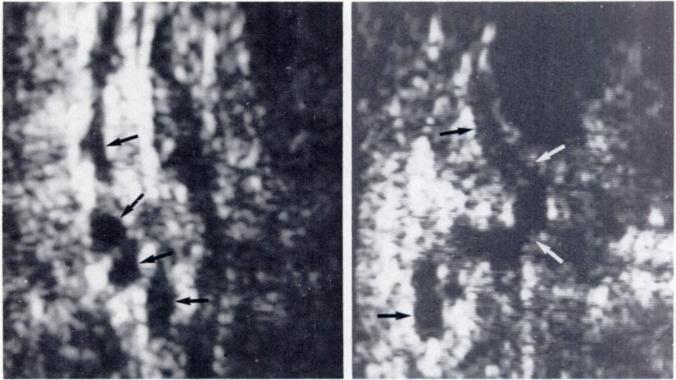
Photo on the left shows normal-sized (1 -1 .5 mm caliber) pampiniform plexus veins (arrows). Right photo shows a single normal vein coursing vertically (arrows) in the proximal spermatic cord.

Left photo shows several loops of dilated veins (small varicocele) about 2-3 mm caliber. Right photo shows large varicocele, with veins measuring 4-5 mm diameter.
Other diagnostic tools include:
- CT scan is useful in showing dilated clusters of enhancing serpentine veins.
- MRI may detect a varicocele incidentally and may show dilated serpentine veins with flow enhancement.
- Venography is only performed during vascular treatment. It may show dilated veins and retrograde blood flow.
Grading of varicocele can be done to describe the severity of the condition:
- A grade 1varicocele shows no dilation of the intrascrotal veins, but with reflux (retrograde/backward flow) in the veins of the spermatic cord in the groin region during a Valsalva maneuver.
- A grade 2varicocele shows prominent veins at upper portion of the testis with reflux during a Valsalva maneuver.
- A grade 3varicocele shows no major dilatation of veins in the supine position, but veins appear dilated up to lower portion of the testis in standing position. Reflux of blood flow is seen at the veins in the lower pole during a Valsalva maneuver.
- A grade 4varicocele shows dilation of veins even when in supine position with reflux during a Valsalva maneuver.
- A grade 5varicocele consists of dilated veins with reflux observed even without a Valsalva maneuver.
What Causes Varicocele?
Varicocele is a fairly common condition, which is seen in about 15 percent of men. It typically develops in adolescence and is likely reduced sperm production. It is also commonly associated with infertility, being found in about 40 percent of affected men.
Varicoceles are classified as either primary or secondary:
Primary varicoceles result from the congenital absence or incompetence of valves in the testicular or internal spermatic vein. This condition usually affects the left testicle.
A secondary varicocele results from increased pressure in the testicular vein, which may be due to compression, obstruction, or a disease associated with portal hypertension.
Varicocele Treatments
Treatment of varicocele is not always necessary, except if it causes pain, reduction in testicular size (atrophy), and infertility.
Surgical treatment aims to seal off affected veins to redirect blood flow into the normal veins. In case of infertility, treatment may improve a man’s ability to produce quality sperm.
Risks associated with repair of varicocele may include:
- Hydrocele or buildup of fluid around your testicles
- Recurrence of varicocele
- Atrophy (shrinkage) of the testicles
- Damage to a blood vessel
- Infection
Surgical repair techniques include:
- Open surgery, under general or local anesthesia. This outpatient procedure involves making an incision in the groin, below the groin, or in theabdomen.
- Use of a surgical microscope, which improves the surgeon’s view during surgery. Another technique involves the use of Doppler ultrasound as guide during the procedure. These techniques are associated with high success rates.
- Laparoscopic surgery involves the use of a thin instrument with a camera, which is inserted through a tiny skin incision in the abdomen. This procedure is done under general anesthesia.
- Percutaneous embolization is an outpatient procedure, which is done under local anesthesia. It involves the insertion of a long tube into a vein in the groin or neck, which is used to pass instruments. Enlarged veins are viewed on a monitor, and the surgeon releases a solution or coils that cause blockage in the dilated testicular veins, thus interrupting blood flow and repairing the varicocele. This procedure is less commonly used.
After the surgery, you will be advised to rest and avoid doing strenuous activities for at least two days. Post-operative pain is usually mild and can be relieved with over-the-counter painkillers. You may also be advised to avoid sex temporarily.
Lifestyle and Home Remedies
Not all varicoceles need surgical treatment, so if you have one that causes minor discomfort, but does not affect fertility, just try using OTC pain relievers such as acetaminophen or ibuprofen. You can also relieve pressure by using and athletic supporter during your activities.
