When the heart rate goes beyond hundred bpm (beats per minute) in adults, it is considered that they are in tachycardia. Tachycardia is a condition in which the heart rate is abnormally high. Tachycardia does not affect adults only and is found in children as well. However, since the standard heart rate continues to vary with age in pediatrics, decision of tachycardia in children depends on the child’s age. There is always an underlying cause when the heart beats too fast though the symptoms, like fussiness, are usually not specific in children.
Normal Heart Rate in Children
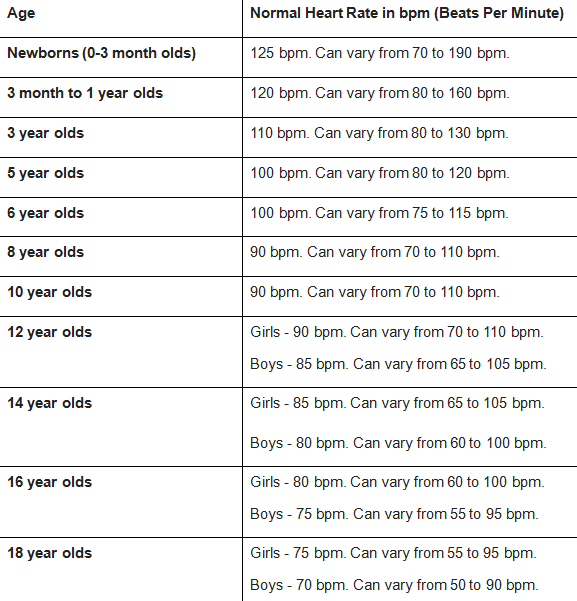
The normal average heart rate of children is higher than that of adults. A heart rate of 60 to 100 bpm when resting is considered normal for adults. The variation in heart rates of children is greater with heart rates varying from 60 bpm (when they are asleep) to 220 bpm (when they are active physically in strenuous activities).
What Is Tachycardia in Children?
The definition of tachycardia in children depends on the age well as on the nature of physical activity the child is doing. A newborn child goes into tachycardia if the heart rate is over 160 bpm while resting. A teenager goes into tachycardia if the heart rate is over 90 bpm while resting. The same teenager won’t go into tachycardia until the heart rate goes over 200 bpm while exercising.
Causes of Tachycardia in Children
Tachycardia can be caused as a result of any physiological process that changes the pattern of sympathetic and parasympathetic innervations received by the heart (sympathetic innervations enhance the heart rate while parasympathetic innervations lower the heart rate). It can also be caused due to an arrhythmia of any type. Arrhythmias that cause tachycardia include like atrial fibrillation and atrial flutter.
Medications can be responsible for causing tachycardia in children too. They do so either through induction of arrhythmia or through the discharge of catecholamines.
Sinus tachycardia (a normal increase in heart rate) is usually occurs due to excitement, physical activity or fever. The increase in heart rate is not alarmingly high and normalcy returns without treatment. In a few rare cases, diseases like high thyroid activity or anemia end up causing tachycardia. In such a case, the treatment of the disease solves the problem of tachycardia too.
Supraventricular Tachycardia (SVT): The Most Common Tachycardia in Children
SVT (Supraventricular Tachycardia) is the most common tachycardia in children.Also known as PSVT (Paroxysmal Supraventricular Tachycardia) and PAT (Paroxysmal Atrial Tachycardia), the condition isn’t considered a serious life threat for young children. The upper and lower heart chambers are involved in the quick heart rate induced by this condition. Doctors only call for treatment if the tachycardia episodes are either too common or too prolonged. Treatments often prove effective with the symptoms stopping after the first six to twelve months of treatment.
In Newborns and Infants
Supraventricular Tachycardia can occur in children of all ages. The condition is capable of affecting newborns and young infants who have completely normal hearts. Among infants, an episode of SVT can take the heart rate to over 220 bpm. Infants become more sleepy and more fussy than normal during an episode of SVT and start to breathe very quickly too. Early diagnosis and treatment of the episode is necessary to restore normalcy. Once the episode is controlled, the infant would be given medications to stop any further recurrences. It is possible that a baby’s heart beats quicker than normal while being in the womb. If the condition is diagnosed at such a point, the mother is given medications which would slow down the heart rate of the child.
In Older Children
In children who are slightly grown up, SVT is accompanied with symptoms like general weakness, pain in the stomach, palpitations, nausea, dizziness and a slight discomfort in the chest region. Children can be taught to control their heart rate with a technique known as Valsalva maneuver. In this technique, the child simply needs to close the mouth and the nose and then make an effort to breathe out.
As compared to newborns and infants, children who are older often suffer from greater number of tachycardia episodes. This is why older children need to be tested more often and need to be treated for longer periods. Neither the episodes nor the tests and treatments should stop the children from living a normal life. The children might need to visit the doctor more often than normal but otherwise; there is no way in which the child’s life would be affected due to SVT.
Treatments
The treatment of SVT consists of two phases. The first phase involves steps taken in order to stop or control the current attack of tachycardia while the second phase involves steps to prevent any further recurrence.
A few easy procedures can prove very effective in ending a given episode of tachycardia. One such procedure is the use of intravenous medications. Catheters (very thin and flexible tubes) can also be used for stopping SVT. In this treatment, the catheter needs to be passed from the nostril to the child’s esophagus and then a very minute current is passed through the catheter in order to control the SVT. A low intensity electrical shock to the wall of the child’s test is another way of controlling SVT.
Treatments to ensure that there is no recurrence of another episode depends entirely on the age of the child. While children above the age of three don’t need to be admitted for the purpose, infants are often kept at the hospital with tests done in order to consistently monitor the effectiveness of the treatment.
Taking Care of the Child after a SVT Episode
It is likely that you would become paranoid about your child’s health after a SVT episode. While it’s normal for you to be so vigilant, you must learn to let your child live normally. It’s best to check your child every now and then but there is no need to stand guard over the child all the time.
It’s best to simply have the telephone number for calling an ambulance saved in your phone so that you can call for one in case an SVT attack lasts for more than half an hour. You should also inform the child’s teacher and babysitter (if there is one) about the condition so that they can take relevant action if the baby suffers from an episode in front of them.
Other Types of Serious Tachycardia in Children
Wolff-Parkinson-White Syndrome
Wolff-Parkinson-White Syndrome, also called the WPW syndrome, is named after the three scientists who discovered the presence of an unusual conduction pathway that connects the ventricles to the atria. The presence of such a pathway leads to a quicker arrival of electrical signals than normal at ventricles.
The WPW syndrome usually shows no symptoms though people with the condition remain under the threat of an abrupt cardiac arrest. The condition can be diagnosed through an ECG. Treatment through medications often proves effective for WPW syndrome. In cases where medications don’t work, more tests are required with the main option being the removal of the pathway via surgery.
Ventricular Tachycardia
Ventricular Tachycardia is a rather rare condition which can be life-threatening in children. It starts in the lower chambers (ventricle)and the main cause of VT is often a severe heart disease.
Specialized tests, like intracardiac electrophysiological procedure, are done in order to understand the severity of the tachycardia. In some cases of VT, there is no treatment required. When treatment is needed, the medications often target the root cause and once the cause gets treated, VT goes away on its own. In cases where medications prove ineffectual, surgery or radiofrequency ablation becomes necessary.
