Endometriosis is a common female problem that is often treated by surgical removal of the uterus (hysterectomy) partially or totally. However, with concerning the recurrence after surgery, non-surgical or laparoscopic treatment must be considered first before deciding to have a hysterectomy. Can endometriosis after hysterectomy recur? How can you prevent? Here we will figure out the answers for you.
What Is Endometriosis?
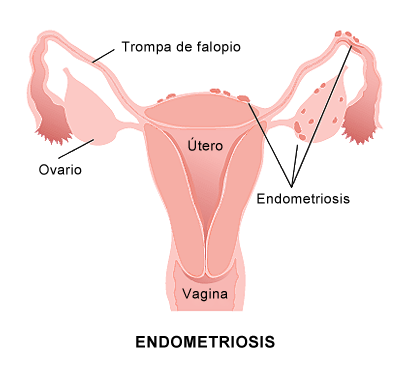
Endometriosis is a painful disorder where tissues normally found lining the inside of the uterus—the endometrium, grow outside the uterus. Endometrial implants may be found in the ovaries, bowels or other tissues lining the pelvis. The displaced endometrial tissues continue to act like the uterine lining and thicken, break away and bleed with every menstrual cycle. However, in endometriosis, since these tissues are trapped outside the uterus, they cannot get out of the body.
Endometriosis can cause severe pain especially during menstrual periods. Fertility problems can also develop. Fortunately, there are various effective medical and surgical treatments.
Can Endometriosis After Hysterectomy Recur?
Yes, the endometriosis after hysterectomy can recur, and the hysterectomy cannot guarantee a cure for endometriosis.
As one of the common treatment options for endometriosis, surgical removal of the uterus (hysterectomy) is reported that pain and other symptoms of endometriosis may recur, where a second operation is needed to remove endometrial implants that develop in other parts of the pelvis.
Another surgical method includes the removal of the ovaries (oophorectomy) during a hysterectomy for women with endometriosis. Some studies show that this treatment method has better results than just a hysterectomy, and fewer women needing a second surgery to treat endometrial implants. The problem, however, with this method is that it may cause premature menopause in young women. That may be because that the ovaries produce hormones that are responsible for maintaining secondary female features and hormonal balance. To avoid premature menopause, hormone replacement therapy would be necessary.
Symptoms of Recurring Endometriosis After Hysterectomy
Endometriosis after hysterectomy usually manifests as pelvic pain, and vaginal or rectal bleeding. Low back pain and pain during sex and defecation are also common problems. To diagnose this condition, your doctor needs to take a second look into your pelvis, which is usually done through laparoscopy—a procedure that involves inserting a long, thin instrument through small cuts in your skin. Fortunately, there are some ways you can try to prevent the recurrence of endometriosis after hysterectomy.
How to Prevent Endometriosis Recurrence
There are certain options for you to prevent recurrence of endometriosis, including hormonal treatment and diet modification.
1. Limit Your Ovulation
Some studies suggest that preventing ovulation helps reduce the risk of recurrenceof endometriosis. This can be done by using oral birth control and hormone replacement therapy using Lupron or others like progesterone/progestin. New findings also show that using an intrauterine device or IUD after surgery may be effective in treating endometriosis and potentially preventing recurrence. Other women choose treatments using an aromatase inhibitor, which stops the production of the female hormone estrogen and minimizes the risk of endometriosis recurrence.
2. Adjust to an Endometriosis Diet
Since estrogen stimulates endometrial growth, this concept advocates avoiding foods that could increase estrogen levels. Also, foods containing plant estrogen (phytoestrogens) or "bad" prostaglandins which can be converted to estrogen should be avoided.
- Turn to vegetables and fruits: Some researchers have found connections between endometriosis and diet high in red meat and low in vegetable and fruits. Therefore, fill your fridge with fruit and vegetables, and reduce the rate of meat of your diet. Add fiber to your diet, which can help to relieve bloating and reduce the estrogen levels. Good sources of fiber are bananas, broccoli, spinach, brown rice, oatmeal, nuts (e.g. almonds, walnuts), etc.
- Take omega-3 fatty acids. Omega-3 fatty acids contain "good" prostaglandins that can help to kill the endometrial cells which can be drained out the body as discharge. This supplement can be quite essential for people with endometriosis.
- Avoid alcohol, caffeine, refined sugar, and fried food. These foods can make your endometriosis symptoms become worse or even aggravated. Also, women with such diet habits are under higher risk of infertility.
NOTE: It is best, however, to talk to your doctor before making significant diet changes, which might lead to other health issues.
3. Boost Immune System
It is also believed that endometriosis may be an autoimmune disorder that could be improved by boosting their immune system. They advocate using supplements that can improve immune system function and prevent endometriosis recurrence. Some studies suggest that fish oil and omega-3 fatty acids may be beneficial. However, more research is necessary regarding the benefits of supplements on endometriosis recurrence. Talk to your physician about using supplements for endometriosis after hysterectomy.
Other Possible Risks of Hysterectomy
Aside from the recurrence of endometriosis after hysterectomy, there are some other possible risks of hysterectomy. Like any other operation, you doctor will inform you of both minor and serious risks that may be involved, although some are not very common.
- Infections: The infections may occur in the area of surgery or even in the lungs or urinary system. To avoid this, surgeons usually administer prophylactic antibiotics before and after the surgery.
- Bleeding or formation of blood clots: There is also a risk of bleeding or formation of blood clots after surgery. Blood clots can travel to the lungs and cause complications like pulmonary embolism. Pressure stockings and medications like heparin can be applied to prevent formation of blood clots; besides, encouraging early ambulation after surgery also helps.
- Damage to some internal structures like the bowels, the bladder or the ureters, which are in the pelvic area may occur, but these are rare complications.
